Taking a stand
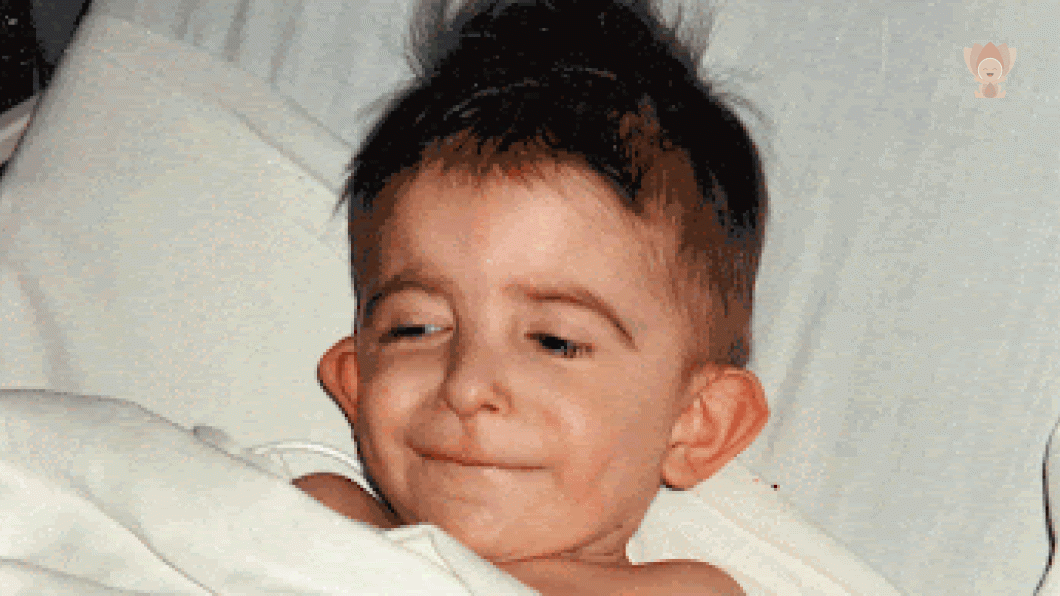
This morning I watched this CP24 story about the fourth time an Ontario mom’s toddler son has had his heart surgery cancelled. Twenty-five years ago, I had my own experience of this with my son, but with a much less frightening surgery: he was getting a g-tube. While waiting for my son’s surgery, I met a mother of a boy who was going in for a major, risky operation. She told me her son had been fully prepared for the operation a couple of days prior, when it was cancelled due to a nursing shortage. Shortly thereafter I found myself holding my sleeping son in our surgeon’s office. Across the hall, I could see the nurses and doctors waiting around the table for him. That’s when our surgery was called off.
By Louise Kinross
At last, he sleeps. He floats. His chest fills and empties. His extravagant eyelashes flicker over a dream. He is still.
We’ve been at the hospital for six hours. Earlier, when nurses struggled to stick an IV into his thread-like veins, he screamed and swung his small, weak arms. D’Arcy and I held him down while they pricked at him, again and again, each poke a stab in my heart.
“It’s okay Ben.”
“I love you Ben.”
“Ben. You need the IV for the operation!”
Now, he lies like deadweight in my lap. He’s four, but the size of a two-year-old. We breathe in tandem, in and out.
Through a glass window I can see the nurses and doctors in the operating room on the other side of the hall.
My son, Ben, has a rare genetic condition called Langer-Giedion syndrome, a random deletion of two genes that probably occurred during cell division. In addition to unusual facial features and protruding ears, he struggles to hear, walk, and speak. We’re in the hospital because he’s stopped growing. Doctors call it “failure to thrive.” Despite a high-fat diet and months of recording every morsel that passes his lips, he’s only 27 lbs.
He’s here to have a hole punctured in his stomach so that an artificial feeding tube, known as a gastrostomy – or g-tube, can be placed. It’s hoped that nighttime feeds will kickstart his growth. To try to make this palatable to Ben, we explained that he would be getting a new belly-button – he would have two!
Twice, the surgery was cancelled the day before scheduled because of a nursing shortage at the children’s hospital.
The second time I called the patient advocate. “Do you know how traumatizing it is to prepare our four-year-old son for this surgery? We’ve booked off work and arranged care for our two-year-old daughter. What am I supposed to tell my son?”
It’s always been hard for me to speak out. I grew up in a British family that was concerned about manners and appearances. My Dad came from a long line of Scotsmen who never complained. I had a wobbly sense of self that relied heavily on the images others held of me. I wanted to be liked. As a result, I smoothed things over when there was a problem. I respected authority and didn’t rock the boat.
That didn’t bode well when I gave birth to a child who was medically compromised.
When Ben was only a day old, a nurse came to my hospital room and lifted him out of my arms. Speechless, I trotted down the hall behind her and into the clinic room, where the pediatrician waited.
“The doctor wants to look at him,” she finally explained – motioning me to the door.
“Alone.”
I walked back into the hall and the doctor slammed the door.
When Ben was close to a year, he developed torticollis – the muscles were too strong on one side of his neck, causing him to sit with his head in a perpetual tilt. “Ben has a rare genetic condition,” I said, as we introduced ourselves to the new therapist assessing him.
“I can SEE that,” she chortled.
Ten days later, as Ben lay on an examining table charming a handful of medical students, the surgeon who was to bring down his testicles pranced into the room and demanded angrily: “What is WRONG with his head?”
I explained that he was born with a head circumference in the 50th percentile, but height below the 3rd, making him look like a little Buddha. He’d already had an ultrasound to rule out hydrocephaly. “What about mental,” the surgeon continued, using his own shorthand for mental retardation. “What about mental?”
The implication that my son was imperfect, flawed, deformed – and lack of the most basic respect for him as a human being – could send me reeling with rage and grief for days. But I didn’t say anything.
Now, I have a four-year-old disabled son who can’t speak. I am the only voice he has. So I call the patient advocate to complain about the cancelled surgery. She says the surgeon will call me, but he never does.
Instead, the surgery is rebooked a third time. Finally, the day arrives.
Ben is sprawled over my lap, hooked up to the IV pole and mercifully, after hours of misery, in a deep sleep. D’Arcy has gone to grab a coffee. We’ve graduated from the waiting room to the surgeon’s inner sanctum, an office directly across from the operating room where he’s giving me final instructions.
There’s a tap at the door. A nurse sticks her head in, wide-eyed. “I need to talk to you,” she says to the doctor.
The doctor leaves, closing the door. Seconds later, he’s back. “I’m sorry, but your son’s surgery has been cancelled,” he tells me.
The words are so unbelievable that at first they hang in the air, like icicles.
“What?”
“There aren’t enough nurses on the floor upstairs.”
I look over at the OR and the expectant faces waiting around the table for my boy. I look down at my son.
I picture us taking him home, trying to explain when he wakes up that the surgery never happened. I imagine telling him that we have to do it all over again: nothing to eat or drink that day; the bungled IVs and pain in his bruised arm; the undignified barium up his bottom; the hours of waiting.
I feel the heaviness of his weight sink into me, the lack of resistance, the letting go.
I’m trapped. I can’t do this to my son.
“I am not moving until my son has his surgery,” I say, speaking with a force that surprises me. “I am not getting up, I am not going home. I am not going to put him through this again.”
We sit in silence. Hot tears gather behind my eyelids. I look into his eyes and I can tell he is a good man.
“Let me see what I can do,” he says. He picks up the phone and calls a senior executive.
“Thank you,” I mouth, as the tears trickle down my face.
The surgeon overrides protocol. Ben goes to the operating room and I go to the waiting room.
I feel depleted and strangely giddy, powerful.
My son may never speak. But he’s given me a voice.
Like this story? Sign up for our monthly BLOOM e-letter. You’ll get family stories and expert advice on raising children with disabilities; interviews with activists, clinicians and researchers; and disability news.
















Leave a comment